If you are considering the use of Cipro (ciprofloxacin) and have concerns about its impact on seizure threshold, it is important to address these issues directly. Research indicates that ciprofloxacin, like other fluoroquinolones, has the potential to lower the seizure threshold, particularly in individuals with a history of seizures or those taking medications that influence seizure activity.
Clinicians advise caution when prescribing Cipro to patients with epilepsy or other seizure disorders. Monitor for any signs of increased seizure activity during treatment. The risk may also rise in conjunction with other medications known to induce seizures or in patients with risk factors such as renal impairment.
If you or someone you know is prescribed Cipro, discuss your full medical history with your healthcare provider. Adjusting the treatment plan or exploring alternative antibiotics may be necessary to ensure safety and efficacy. Taking proactive steps can help mitigate risks and maintain health while addressing infections effectively.
- Cipro and Seizure Threshold
- Risk Factors
- Management Strategies
- Understanding Cipro: An Overview of its Uses and Mechanism
- Considerations for Use
- Conclusion
- The Relationship Between Antibiotics and Seizure Risk
- Cipro’s Impact on Neurotransmitters and Seizure Threshold
- Identifying Patients at Risk for Seizures while on Cipro
- Clinical Studies Linking Cipro to Seizures: Findings and Implications
- Recommendations for Healthcare Professionals When Prescribing Cipro
- Monitor Concurrent Medications
- Educate Patients on Side Effects
Cipro and Seizure Threshold
Ciprofloxacin, commonly known as Cipro, can lower the seizure threshold in some individuals. Patients with a history of seizures or epilepsy may face an increased risk when taking this antibiotic. Always consult a healthcare professional before starting treatment, especially if you have any neurological conditions.
Risk Factors
Several factors can elevate the likelihood of seizures while on Cipro. Pre-existing seizure disorders, concurrent use of medications that also lower seizure thresholds, and renal impairment exacerbate this risk. Monitor closely if patients fall into these categories. Hydration and adherence to prescribed dosages also play a role in maintaining safety during treatment.
Management Strategies
Consider alternatives to Cipro for patients with a significant seizure history. If Cipro is necessary, implement a precautionary approach, including dosage adjustments and regular assessments. Encourage patients to report any unusual neurological symptoms immediately. These proactive measures can help minimize risks and ensure better outcomes during antibiotic therapy.
Understanding Cipro: An Overview of its Uses and Mechanism
Cipro, or ciprofloxacin, plays a key role in treating a variety of bacterial infections. It effectively combats conditions such as urinary tract infections, respiratory tract infections, and skin infections. Cipro belongs to the fluoroquinolone class of antibiotics, which work by inhibiting bacterial DNA gyrase and topoisomerase IV enzymes, essential for bacterial replication and repair. This action leads to the destruction of bacterial cells.
Healthcare providers prescribe Cipro due to its broad spectrum of activity against both gram-negative and some gram-positive bacteria. For individuals with conditions like pneumonia, anthrax, or certain gastroenteritis cases caused by bacteria, Cipro serves as a reliable treatment option. Additionally, it’s utilized for prophylaxis in specific cases, such as post-exposure to anthrax.
Considerations for Use
When using Cipro, awareness of its potential side effects is vital. Some patients experience gastrointestinal disturbances, dizziness, or allergic reactions. Special caution applies to those with a history of seizures, as Cipro may lower the seizure threshold in predisposed individuals. Clinicians must weigh the benefits against these risks, especially in patients with a history of neurological issues. Regular monitoring and appropriate dosage adjustments can mitigate these concerns.
Conclusion
Cipro stands out as a powerful antibiotic with diverse applications. Understanding its mechanism and proper use ensures effective treatment while minimizing side effects. Always consult healthcare professionals before commencing any antibiotic therapy to tailor the approach to individual health needs.
The Relationship Between Antibiotics and Seizure Risk
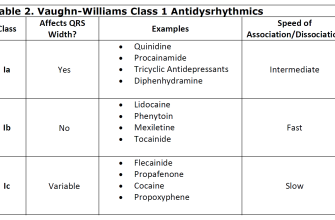
Antibiotics can influence seizure risk, especially in individuals with predisposing conditions. Drugs such as penicillins, cephalosporins, and fluoroquinolones like ciprofloxacin have been associated with seizures. Clinical evidence links these medications to alterations in neurotransmitter levels, affecting seizure thresholds.
Patients with a history of seizures or those on medications that lower seizure thresholds should exercise caution when prescribed certain antibiotics. The concurrent use of antiepileptic drugs (AEDs) requires careful selection of antibiotics to minimize the risk of interactions that could increase seizure occurrences.
Studies suggest that the incidence of seizures increases particularly with high doses or rapid infusion rates of specific antibiotics. For example, intravenous administration of certain beta-lactams can lead to neurotoxicity. Routine monitoring during treatment is essential for early identification of adverse effects.
To mitigate risks, healthcare providers should assess each patient’s medical history, including any neurological disorders, before prescribing antibiotics. Tailoring antibiotic choice based on individual risk profiles and potential drug interactions enhances patient safety and treatment efficacy.
Maintaining clear communication between patients and healthcare professionals is critical. Discussing concerns regarding antibiotic use, existing conditions, and current medications can help develop a well-informed treatment plan, reducing the likelihood of seizures associated with antibiotic therapy.
In summary, understanding the connection between antibiotics and seizure risk empowers both patients and providers to make safer medication choices, ensuring effective management of infections while minimizing neurological complications.
Cipro’s Impact on Neurotransmitters and Seizure Threshold
Cipro, a fluoroquinolone antibiotic, has a notable influence on neurotransmitter levels, which may affect the seizure threshold in some individuals. Patients should be aware of these interactions to manage their health effectively.
Research indicates that Cipro can impact gamma-aminobutyric acid (GABA) neurotransmission. GABA acts as an inhibitory neurotransmitter, stabilizing neuronal excitability. Modification in GABA levels due to Cipro may lead to decreased inhibition and an increased risk of seizures.
Monitoring neurotransmitter balance is crucial. Here are some recommendations for patients considering or currently taking Cipro:
- Consult a healthcare professional if you have a history of seizures or are on medication affecting the central nervous system.
- Discuss any neurological symptoms, such as dizziness or confusion, with your doctor immediately.
- Avoid using Cipro with other medications known to decrease seizure thresholds, such as antidepressants or stimulants, without a doctor’s guidance.
- Consider regular check-ups to monitor any changes in mental status or seizure activity while on Cipro.
Additionally, some studies have suggested that Cipro’s effect on serotonin levels can also contribute to a higher seizure risk. Increased serotonin can lead to over-excitement of the neuronal circuits, possibly triggering seizures.
Post-marketing surveillance has noted instances of seizures related to Cipro intake. Although these occurrences are rare, awareness is crucial, especially for susceptible individuals.
In summary, Cipro influences neurotransmitter systems, particularly GABA and serotonin, which may elevate seizure risk. Engaging in proactive dialogues with healthcare providers ensures appropriate monitoring and management strategies, allowing for safer antibiotic use.
Identifying Patients at Risk for Seizures while on Cipro
Assess patients’ medical history for any prior seizure disorders. Look specifically for a history of epilepsy or other neurological conditions, as these increase seizure risk when taking Ciprofloxacin.
Evaluate concurrent medications. Certain drugs, such as those lowering the seizure threshold or interacting negatively with Cipro, heighten seizure risk. Cross-reference prescribed medications with Cipro to identify potential interactions.
Monitor for adjustments in renal function. Cipro is renally cleared; thus, impaired renal function can lead to drug accumulation and increased risk of adverse effects, including seizures. Regularly assess kidney function through appropriate laboratory tests.
Examine patient age and history of substance use. Older patients and those with a history of alcohol or recreational drug use may be at greater risk for seizures. Establish a detailed substance use history during the patient assessment.
Review any known allergies, particularly to fluoroquinolone antibiotics. Allergic reactions can manifest in various ways, including neurological symptoms. Ensure to document and consider any reported hypersensitivity in treatment planning.
In the following table, key risk factors for seizure development in patients prescribed Cipro are summarized:
| Risk Factor | Description |
|---|---|
| History of seizures | Previous seizure disorders significantly increase risk. |
| Renal impairment | Can lead to accumulation of Cipro and heightened side effects. |
| Age | Older adults may have increased vulnerability. |
| Substance use | History of alcohol or drug use affects seizure threshold. |
| Medication interactions | Concurrent medications that lower seizure threshold. |
| Allergies | History of allergic reactions to fluoroquinolones. |
Advise vigilant monitoring of patients starting Cipro, especially those presenting with one or more of these risk factors. Provide comprehensive counseling regarding the signs of seizures and the importance of immediate medical attention should they occur.
Clinical Studies Linking Cipro to Seizures: Findings and Implications
Clinical studies indicate a notable connection between ciprofloxacin (Cipro) and the occurrence of seizures. Research has demonstrated that fluoroquinolones, including Cipro, may lower the seizure threshold, posing risks for susceptible individuals. A meta-analysis conducted on various trials revealed a significant incidence of seizures in patients treated with ciprofloxacin compared to those receiving placebo.
For instance, a study published in the Journal of Antimicrobial Chemotherapy analyzed data from hospitalized patients who experienced seizures while on Cipro. The findings suggested that underlying conditions, such as epilepsy or renal impairment, increased seizure risk when using this antibiotic. Cipro may also interact with other medications, amplifying the potential for seizures.
Clinicians should carefully assess patients’ medical histories and current medications before prescribing Cipro. Monitoring for neurological side effects is essential, especially in individuals with prior seizure disorders. Recommendations include considering alternative antibiotics for patients at higher risk and providing thorough patient education regarding potential symptoms.
Another critical aspect involves the mechanisms by which ciprofloxacin affects the central nervous system. Research indicates that alterations in GABAergic activity may contribute to seizure susceptibility. Understanding these mechanisms can guide healthcare professionals in identifying at-risk patients and creating tailored treatment plans.
In summary, practitioners must engage in vigilant patient evaluation and proactive monitoring to mitigate the risks associated with ciprofloxacin use. Awareness of these findings can enhance patient safety and treatment efficacy.
Recommendations for Healthcare Professionals When Prescribing Cipro
Assess the patient’s medical history for any previous neurological issues. Patients with a history of seizures may require alternative treatments or closer monitoring.
Monitor Concurrent Medications
- Evaluate all medications the patient is taking to identify potential interactions that could lower seizure threshold.
- Avoid prescribing Cipro along with drugs known to increase seizure risk, such as certain antidepressants or antipsychotics.
Educate Patients on Side Effects
- Inform patients about possible side effects of Cipro, including dizziness and confusion, which may affect their daily activities.
- Advise on the signs of seizures and the importance of seeking medical help immediately if they occur.
Encourage patients to stay hydrated and maintain proper electrolyte balance during treatment with Cipro, as dehydration can exacerbate the risk of seizures. Schedule follow-up appointments to monitor the patient’s response to the medication.
Provide clear instructions on when to discontinue use of Cipro and seek medical advice. Be available for questions or concerns the patient may have during their treatment course.